What is Optimal Outpatient Appointment Scheduling?

For medical centers, appointment scheduling is part of delivering high-quality care. Learn more about optimal outpatient appointment scheduling…
Each day, healthcare centers serve a massive number of patients with varying medical needs. As a result, healthcare administrators must maintain a delicate balance to ensure patients don’t miss appointments or crowd waiting rooms.
Every patient follows a different path from diagnosis, pharmacy, scans, consultation, etc. throughout each department in a medical center. Poor outpatient resource scheduling can either result in idle time for hospital staff or overstretching the limited number of healthcare providers.
That said, an optimized scheduling system is beneficial to the workforce, finances, and patient satisfaction.
What is Optimal Outpatient Appointment Scheduling?
The objective of optimal outpatient scheduling is to decongest waiting rooms, minimize staff pressure, and enhance patient satisfaction. Negative consequences of poor scheduling include excessive overtime that can lower staff morale or affect productivity. Congested waiting rooms pose health risks to your staff and impact your brands’ reputation.
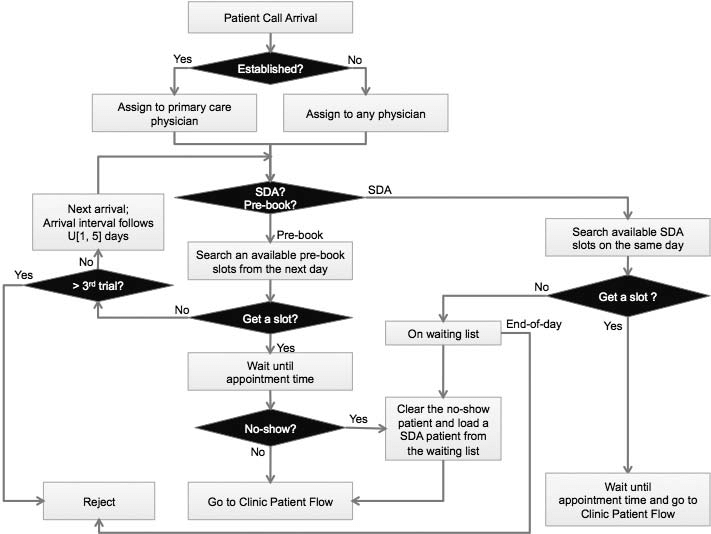
Optimal outpatient appointment scheduling may include a patient scheduling workflow that looks like:
By mapping out the possible scenarios and required actions at each step of the patient scheduling journey, healthcare centers can effectively optimize scheduling and work towards a lean, efficient scheduling process.
Below are a few improvement scenarios aimed at dealing with congestion.
- Reschedule patients from congested to less congested areas: One of the direct impacts is reduced congestion at peak hours or routines. The technique has influenced the present design, which tries to schedule an appointment in time blocks that impact the existing infrastructure and staff.
- Service locations: Another interesting methodology is to have patients wait in different service areas besides the typical waiting room. Dispatching patients in other locations help hospitals deal with the urge to hire an extra nurse or doctor.
Four ways to achieve Optimal Outpatient Scheduling
1. Embrace patient self-scheduling technology
A significant percentage of patients prefer technology solutions like apps and online systems to book appointments or schedule a hospital visit. Find a system that is patient and user-friendly to bring more people on board. Such a solution reduces the time and staff required to book appointments, send reminders and documentation.
2. Minimize scheduling restrictions
The administration can work on ways to minimize appointments that can only be executed at a specific time or day— such as physician clinics. Some administrators fear minimal restriction because of potential congestion; however, complex situations and demands are evenly distributed.
3. Create standardized appointment times
It’s essential to understand the total time a patient can take while waiting to be served. The understanding forms a basis to design standard appointment duration, for example, 15, 20, or 30 minutes. On the other hand, a patient that spends little time with a doctor leaves room for others with complex issues — creating a balance.
4. Closely monitor appointments
The administration should also address appointment issues such as lateness or no-shows. One option is creating a waiting list to replace such patients. Alternatively, the administration can leverage technology to create timely reminders via email or text. You can include a statement that prompts patients to confirm attendance or further information — the extra details eliminate uncertainties surrounding appointments.
Contingency plans for Optimal Outpatient Appointment Scheduling
There are frequent outliers in a standard demand curve that can overwhelm a system if not anticipated and planned. Practical scenarios include a sudden spike in demand during the flu season or certain months of the year when workers take a leave or vacation.
Lack of contingency plans may suspend service delivery and quality thereof. It’s crucial to put protocols, roles and plans to deal with the unexpected turn of events. Here are a few items to consider:
Create an agreeable timetable for vacation
Healthcare providers have a right to take a few days off, which causes strain on the remaining healthcare providers. It’s essential to have an agreement with the team on ways to cope with such situations. It can include more patients per healthcare provider, fewer breaks, or synchronizing the vacations to minimize disruptions.
Plan for huge demand
The available healthcare workers can be overwhelmed if a few workers are sick or during outbreaks like salmonella. The management can put measures like suspending physical health checks, call part-time workers, or hiring temporary healthcare providers.
Create a contingency manual
The management can write a contingency manual to guide the workforce during a crisis. These protocols help supervisors, clerks, and officers act quickly without the need to make phone calls.
Why outpatient medical centers should embrace Optimal Appointment Scheduling
- Efficient staff and resource management. A solid appointment plan is a path to efficient utilization of the healthcare workforce. The management can anticipate which periods require extra workers, part-time staff, overtime, or temporary hires. The plan can help allocate sufficient furniture in waiting areas or doctors to prepare with the right supplies and resources for an appointment.
- Improved patient satisfaction. Patients can use an automatic scheduling system to book or adjust appointments remotely. It also eliminates the need to spend long hours in the queue. As a result, there are minimal service complaints which is a reflection of improved service.
- Cost optimization strategy. Optimal out-patient resource scheduling results in better utilization of the workforce, the system, and hospital resources. As such, management decisions such as hiring an extra worker are based on a scientific formula.
Dangers of medical resource downtime
The downtime of equipment is a significant contributor to inefficiencies in productivity. The downtime of an automated system in a healthcare facility can put patients at risk, overwork staff, create idle time and disarray in the entire facility.
Below are some of the consequences of downtime in a healthcare facility.
- Wasted labor: Healthcare providers cannot serve efficiently without systems such as a scheduling system. Therefore, it can result in multiple missed appointments and idle time for healthcare providers — labor paid to workers goes to waste when downtime is frequent.
- Poor patient care: Taking care of patients requires working equipment during emergencies, billing, and inpatient care admission. Frequent downtime affects the speed and smooth sailing of vital operations leading to poor service delivery.
Optimize your patient scheduling processes
Lost productivity, wastage of resources, and bad reputation are some of the adverse effects of unplanned appointment scheduling. Therefore, a healthcare facility should find the perfect balance when dealing with high or low patient numbers with regard to the available healthcare providers.
That said, you can always partner with CCD for a quality patient scheduling solution. We have a history of providing secure, compliant, and modern systems accessible on multiple platforms. Click here to build an optimal appointment scheduling tool.